? What Does “Evidence-Based” Really Mean in Medicine
Raghad Altoubah- Reproductive & Fertility Medical Writer
Imagine you’re sitting in a doctor’s office. You’re worried, hopeful, maybe overwhelmed. The doctor recommends a test, a treatment, or a lifestyle change and says:
“This is evidence-based.” It sounds reassuring. Scientific. Safe.
But what does evidence-based actually mean and why should you care?
Let’s strip away the jargon and get to the truth.

Evidence-Based Medicine: Not Opinions, Not Trends
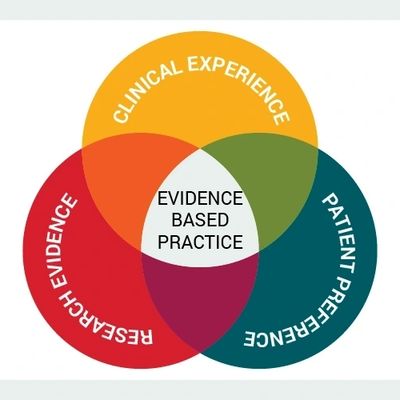
Evidence-based Medicine (EBM) means making medical decisions using the best available scientific evidence, combined with clinical expertise and the patient’s values and circumstances.

That’s it. No magic. No authority-based guessing. No “this is how we’ve always done it.”
The concept was formalized in the 1990s by researchers at McMaster University, and it changed medicine forever.
Before EBM, many treatments were based on tradition, senior opinion, or limited observation. Some worked. Many didn’t. A few caused real harm.
Evidence-based medicine was medicine growing up.
➤ What Counts as “Evidence”?
Not all evidence is equal. One small study or a social media claim does not equal proof.
➜ In evidence-based medicine, evidence follows a hierarchy:
1. Systematic reviews and meta-analyses
These combine results from many high-quality studies. This is the gold standard.
2. Randomized controlled trials (RCTs)
Participants are randomly assigned to groups, reducing bias.
3. Cohort and case-control studies
Useful, but more prone to hidden variables.
4. Expert opinion and case reports
Valuable for ideas, but weakest for decision-making.
If you hear “evidence-based,” the claim should stand on levels 1 or 2, not personal experience alone.
Evidence-Based ≠ One-Size-Fits-All
★ Here’s a blind spot many people miss:
- Evidence does not replace human judgment.
- A treatment can be strongly supported by science and still be wrong for you.
➜ That’s why true evidence-based care always includes:
- Your age and biological sex
- Your medical history
- Your goals (fertility, longevity, quality of life)
- Your values and tolerance for risk
This is especially critical in Reproductive Health and Fertility, where timelines, emotions, and personal priorities matter deeply.
➤ Why Evidence-Based Medicine Protects Patients
Medicine moves fast. New tests, supplements, procedures, and “breakthroughs” appear every week.
➜ Without evidence-based standards:
- Ineffective treatments spread
- Costs rise without benefit
- False hope replaces real outcomes
- Harmful practices go unchecked
Evidence-based medicine acts as a filter, separating:
✔ what sounds good … from … ✔ what actually works
This matters enormously in fertility care, pregnancy, contraception, and hormonal health areas historically filled with myths, stigma, and outdated beliefs.
➤ What Evidence-Based Medicine Is Not
Let’s be clear:
❌ It is not rigid or anti-innovation
❌ It is not “only numbers, no humanity”
❌ It is not ignoring patient experience
In fact, patient-reported outcomes increasingly shape modern research.
Evidence-based medicine evolves as better evidence emerges. Good science changes its mind when the data demands it.
That’s a strength .. not a weakness.
➤ How You Can Spot Evidence-Based Information
Whether you’re reading an NGO website, a health article, or a clinic brochure, ask these questions:
- Are claims supported by reputable studies?
- Are risks and limitations discussed honestly?
- Are absolute benefits explained—not exaggerated?
- Are sources transparent and up to date?
If everything sounds too perfect, it probably isn’t evidence-based.
★ The Bottom Line
Evidence-based medicine is about trust earned, not assumed.
It respects science.
It respects patients.
And it demands accountability from healthcare systems, companies, and professionals alike.
In a world overflowing with health advice, evidence-based medicine is not just a technical term .. it’s a promise:
Your care is guided by knowledge, not noise.
And that promise matters.

.png)