FERTILITY HEALTH | WOMEN’S HEALTH | REPRODUCTIVE AWARENESS
AMH: The Hormone That Tells You About Your Fertility.
A plain-language guide to Anti-Müllerian Hormone! what it means, what it doesn’t, and why it matters.
You might have heard about AMH from a friend who went through IVF, from a social media post, or perhaps a doctor mentioned it during a routine checkup. And maybe, like many people, you walked away with more questions than answers.
That’s exactly why we’re here. Let’s talk about AMH clearly, honestly, and without the fear-mongering.
➤ So, What Exactly Is AMH?
AMH stands for Anti-Müllerian Hormone. It’s a protein hormone produced by small follicles in the ovaries! The tiny sacs that hold immature eggs. The more of these follicles you have, the more AMH your body produces.
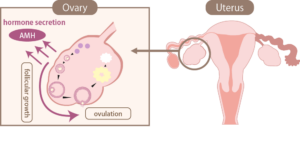
In simple terms: AMH gives doctors a window into your ovarian reserve, the pool of eggs your ovaries still have available.
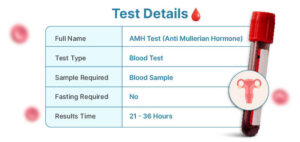
It’s measured through a simple blood test and doesn’t require you to be on any specific day of your menstrual cycle, which makes it a convenient and reliable marker.
💡 Think of AMH as a rough “egg count” indicator. It doesn’t tell you everything, but it gives a meaningful snapshot of where you stand.
➤ Why Does AMH Matter?
Women are born with all the eggs they will ever have, roughly 1 to 2 million at birth. By puberty, that number drops to around 300,000–500,000. And throughout the reproductive years, that reserve keeps declining naturally.
AMH reflects how quickly or slowly, that decline is happening for you personally. It’s one of the most reliable markers we have for ovarian reserve, and it’s widely used in fertility assessments worldwide.
Measuring AMH can help:
- Assess fertility potential before trying to conceive
- Guide decisions about egg freezing (oocyte cryopreservation)
- Help fertility specialists plan IVF protocols
- Detect conditions like Polycystic Ovary Syndrome (PCOS), where AMH is often elevated
- Identify premature ovarian insufficiency (POI), where AMH is very low in younger women
➤ What Do AMH Numbers Actually Mean?
AMH is measured in nanograms per milliliter (ng/mL). Here are general reference ranges, though always interpret these with your doctor, as lab ranges may vary slightly:
Important: These are population averages, not verdicts. A lower AMH doesn’t mean you cannot conceive naturally. It means your egg pool may be smaller, which can make conception take longer or make certain fertility treatments more relevant to discuss.
➤ What AMH Cannot Tell You
This is where misinformation often creeps in, so let’s be very clear.
AMH does NOT tell you:
- Whether your eggs are healthy or genetically normal
- Your exact chance of getting pregnant in any given month
- That you are infertile (a single test never determines this)
- How long you have until menopause
⚠️ A low AMH with a normal menstrual cycle may still mean natural conception is possible. Conversely, a normal AMH doesn’t guarantee easy fertility. Quality and quantity are two different things.
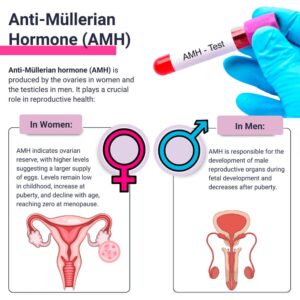
➤ What About Men? Is AMH Relevant?
Yes!! AMH is also produced in the testes during fetal development and early childhood. In adult men, AMH levels are used in specific diagnostic contexts, particularly when evaluating undescended testes, disorders of sex development (DSD), or certain types of male infertility. It is not routinely tested in adult male fertility workups, but it is a recognized marker in pediatric and specialized urology settings.
➤ When Should You Consider Getting an AMH Test?
You may want to discuss AMH testing with your doctor if you:
- Are over 30 and planning to conceive in the next 1–3 years
- Are considering egg freezing as a fertility preservation option
- Have been trying to conceive for 6–12 months without success
- Have a family history of early menopause
- Have been diagnosed with or are being assessed for PCOS
- Are about to undergo chemotherapy or radiation (which can affect ovarian reserve)
- Have had previous ovarian surgery
📋 AMH testing is a starting point for a conversation, not a final answer. Always discuss results with a qualified reproductive specialist or gynecologist.
Can You Improve Your AMH Level?
This is one of the most frequently asked questions and the honest answer is: not significantly through lifestyle alone.
AMH reflects your biological reserve, which is largely determined by genetics. No supplement, diet, or lifestyle change has been proven in high-quality clinical trials to meaningfully raise AMH in women with diminished ovarian reserve.
However, there are good reasons to take care of your overall reproductive health:
- Avoid smoking! it’s strongly linked to accelerated ovarian aging
- Maintain a healthy body weight! Extreme weight loss or obesity can affect hormonal balance
- Limit alcohol consumption
- Manage chronic stress! while it doesn’t directly raise AMH, it supports general hormonal health
Some studies have explored the role of Vitamin D, CoQ10, and DHEA in ovarian function, but evidence remains preliminary. Speak to your doctor before starting any supplement regimen.
A Note on PCOS and High AMH
In women with Polycystic Ovary Syndrome (PCOS), AMH is often significantly elevated — sometimes 2 to 3 times higher than average. This is because PCOS involves an accumulation of small antral follicles, each contributing to AMH production.
Higher AMH in PCOS does not mean “extra fertility.” It reflects a hormonal and follicular imbalance, and women with PCOS often face their own fertility challenges, including irregular ovulation. If you have PCOS, your AMH results need to be interpreted in the full context of your diagnosis.
The Bottom Line
AMH is a valuable, evidence-based tool in Reproductive Medicine. It helps you and your healthcare provider make more informed decisions, whether you’re planning a pregnancy now, in the future, or exploring your options.
But it’s one piece of a much larger picture. Your fertility story is shaped by many factors: age, overall health, partner fertility (if applicable), egg quality, uterine health, and more.
✅ Knowledge is power! but knowledge in context is even better. If you’ve had an AMH test or are considering one, use it as a launchpad for a real conversation with your doctor, not as a reason to panic or celebrate prematurely.
This article is for educational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider for personalized guidance.

.png)