Hormonal Imbalance: What That Term Really Means
Raghad Altoubah- Reproductive & Fertility Medical Writer

Learn what hormonal imbalance really means, which symptoms actually point to a hormonal condition, and when to seek medical support. Evidence-based guide for men and women.
Hormonal Imbalance: What That Term Really Means
“Your hormones are off” is one of the most common things people say when something feels wrong with their body. Fatigue, weight changes, low mood, irregular periods, poor sleep.
Hormones get blamed for all of it. But what does hormonal imbalance actually mean? And when does it go from a vague feeling to something a doctor can identify and treat?
Hormones: A Quick Recap
Hormones are chemical messengers produced by glands throughout your body, including the Thyroid, Adrenal glands, Ovaries, Testes, and Pancreas. They travel through the bloodstream and regulate nearly every major function: metabolism, reproduction, sleep, stress response, and mood.
The Endocrine Society defines hormonal disorders as conditions where glands produce too much or too little of a hormone, or where the body’s cells do not respond to hormones correctly.
This is the clinical meaning of “imbalance” It is a specific, measurable disruption, not a catch-all explanation for feeling unwell.
The Problem With the Term “Hormonal Imbalance”
The phrase is widely used but medically imprecise. In clinical practice, no doctor diagnoses a patient with “hormonal imbalance” alone.
Instead, they identify specific conditions: Polycystic ovary syndrome (PCOS), Hypothyroidism, Hyperthyroidism, Hypogonadism, Insulin resistance, Adrenal insufficiency, and others.
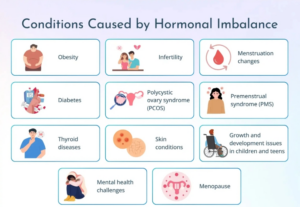
Common Conditions That Involve Hormonal Disruption
Several well-defined conditions reflect true hormonal dysregulation. These are the ones backed by clinical evidence:
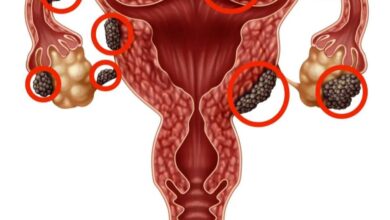
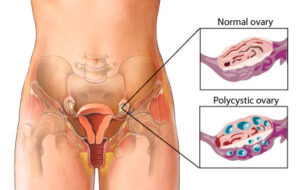
1- Polycystic Ovary Syndrome (PCOS)
PCOS affects 8 to 13 percent of reproductive-age women worldwide, according to the World Health Organization.
It involves elevated androgens (male-type hormones), irregular ovulation, and metabolic changes.
Symptoms include irregular periods, acne, excess hair growth, and difficulty conceiving. It is also linked to insulin resistance.
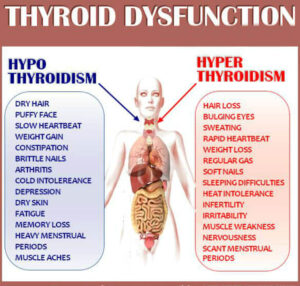
2- Thyroid Disorders
The thyroid gland regulates metabolism through two key hormones: T3 and T4. Hypothyroidism (underactive thyroid) causes fatigue, weight gain, cold sensitivity, and depression.
Hyperthyroidism (overactive thyroid) causes weight loss, palpitations, anxiety, and heat intolerance.
Both are diagnosed through blood tests and are highly treatable.
3- Male Hypogonadism
Low testosterone in men is a recognized clinical condition that increases with age.
The American Urological Association estimates that about 40 percent of men over 45 have low testosterone.
Symptoms include reduced libido, fatigue, mood changes, and decreased muscle mass.
It is diagnosed through blood testing and clinical evaluation.
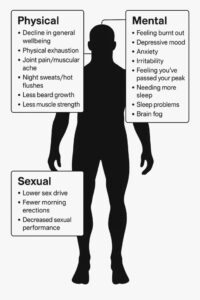
4- Insulin Resistance and Metabolic Hormones
Insulin is a hormone produced by the pancreas.
When cells stop responding to it effectively, blood sugar rises and the body compensates by producing more insulin, Over time, this can lead to type 2 diabetes.
Insulin resistance is closely linked with PCOS in women and with obesity in both sexes.
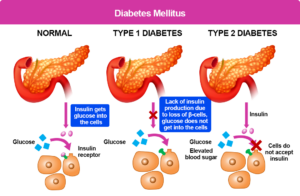
5- Adrenal Disorders
The adrenal glands produce cortisol, the body’s primary stress hormone.
Chronic stress does not “break” the adrenal glands (a concept called adrenal fatigue that lacks scientific validation), but true adrenal insufficiency, such as Addison’s disease, is a serious, diagnosable condition.
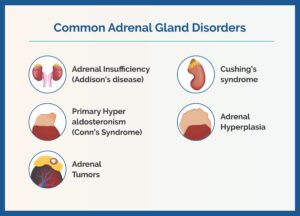
Symptoms That Are Worth Investigating
Not every symptom is hormonal in origin, but the following can be a reason to ask your doctor for an endocrine evaluation:
- Persistent fatigue not explained by sleep quality or lifestyle
- Unexplained weight gain or weight loss
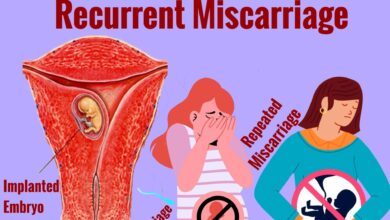
- Irregular, absent, or very heavy menstrual cycles
- Difficulty getting pregnant after 12 months of trying (or 6 months if over 35)
- Significant changes in mood, memory, or concentration
- Excess hair on the face or body (in women)
- Hair thinning or loss
- Low libido or sexual dysfunction
- Persistent acne in adulthood
- Feeling unusually cold or hot
These symptoms on their own are not proof of a hormonal condition.
Many have other causes. But patterns of these symptoms together, particularly if they are new or worsening, are worth a conversation with a healthcare provider.
How Hormonal Conditions Are Diagnosed
Diagnosis relies on blood tests, physical examination, and in some cases imaging.
There is no single “hormonal panel” that checks everything at once. Your doctor will order specific tests based on your symptoms and medical history.
Some important markers include TSH (thyroid-stimulating hormone) for thyroid function, FSH and LH for ovarian or testicular function, testosterone for both men and women, AMH (anti-Mullerian hormone) as a marker of ovarian reserve, fasting insulin and glucose for metabolic assessment, and prolactin, which can affect cycles and fertility when elevated.
What You Can Do
Some lifestyle factors have a meaningful, evidence-based impact on hormonal health:
- Sleep: Poor sleep disrupts cortisol, insulin, leptin, and reproductive hormone rhythms. The National Sleep Foundation recommends 7 to 9 hours for adults.
- Nutrition: A diet high in refined carbohydrates and low in fiber worsens insulin sensitivity. For women with PCOS in particular, dietary patterns matter significantly.
- Exercise: Regular moderate-intensity exercise improves insulin sensitivity, reduces cortisol dysregulation, and supports healthy testosterone levels in men.
- Stress management: Chronic psychological stress activates the HPA axis and maintains elevated cortisol. Evidence supports mindfulness-based practices, therapy, and rest as meaningful interventions.
- Avoiding endocrine-disrupting chemicals: Certain plastics (BPA), pesticides, and synthetic fragrances can mimic or block hormone activity. Limiting exposure is a reasonable precaution.
When to See a Specialist
If your symptoms are affecting your quality of life, fertility, or daily functioning, ask your primary care doctor for a referral to an endocrinologist or, if reproductive concerns are central, a reproductive endocrinologist (REI) or gynecologist with expertise in hormonal disorders.
You deserve a specific answer, not just a vague reassurance that “your hormones are a bit off.”
This article is for educational purposes only and does not constitute medical advice. Please consult a qualified healthcare provider for personalized guidance.

.png)